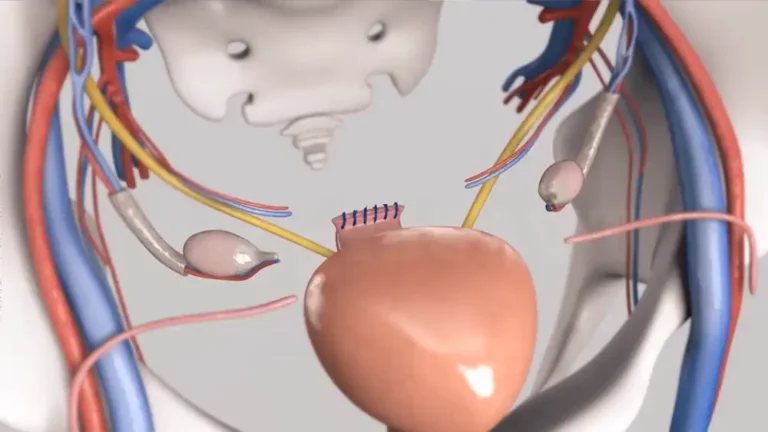
Hysterectomy Recovery: What to Expect at 4 Months
What to expect 4 months after hysterectomy surgery?
If you have recently undergone a hysterectomy, you may be uncertain about what to expect in the months that follow. Even though healing can take some time, the good news is that most women can resume their regular activities within a few months of surgery.
At the four-month mark, you should feel significantly better than immediately after this major surgery. It is essential to remember that everyone’s recovery is different.
Some women may recuperate more slowly than others; therefore, it is essential to pay attention to your body and give yourself the space and time you require to recover.
Incision care after 4 months
Incision care is a crucial component of the post-hysterectomy recuperation procedure. Four months after surgery, your incision site should be completely recovered, but you must continue to monitor it and take care of it to prevent complications.
Following surgery, the incision site may be tender or sore for several weeks. However, with adequate care, you can reduce any discomfort and speed up the healing process.
Be sure to follow your doctor’s instructions for cleansing and caring for your incision site, and refrain from engaging in any activities that could cause strain on the area like heavy lifting.
In some circumstances, even four months following surgery, you might still feel pain or discomfort at the incision site. Pain medication or other treatments that your doctor has recommended can be used to address better pain control.
It’s crucial to keep an eye out for infection symptoms including redness, edema, or discharge at the incision site. Call your doctor right away if you notice any of these signs. To help in the eradication of the infection and the prevention of its spread, they could suggest antibiotics or other treatments.
Resuming normal physical activities
Resuming regular physical activity after a hysterectomy might be challenging. It’s crucial to give yourself ample time to recover before returning to your regular schedule.
Your body should fully heal from surgery in up to six weeks, though some women may require longer. When it is safe to resume particular activities, your doctor will provide you with detailed guidelines.
After a hysterectomy, walking is a fantastic exercise to start with. Additionally to enhancing blood flow, it can aid in preventing blood clots formation. Start off with short walks, then as you get more at ease, gradually increase the distance. It’s critical to pay attention to your body’s signals and avoid overexerting yourself.
Another beneficial workout to attempt after a hysterectomy is yoga. It can aid in enhancing flexibility, lowering stress levels, and encouraging relaxation.
However, you should avoid any poses that require you to twist your torso, generate chest pain or put pressure on your abdomen. Your doctor may advise modified poses or advise delaying your first yoga session until you are fully recovered.
For at least six weeks following surgery (even up to eight weeks), it is best to refrain from heavy lifting and other vigorous activity. This includes carrying out sit-ups, crunches, and any other exercises that heavily utilize the abdominal muscles, such as lifting objects that weigh more than 10 pounds. You’ll be informed by your doctor when it’s okay to resume these activities.

It is important to be patient with yourself during the recovery period. Your body has been through a lot and it takes time to heal fully. Celebrate small milestones along the way and don’t be too hard on yourself if you experience setbacks.
Specific outcomes for different types/techniques
Patients might anticipate noticeable enhancements in their quality of life four months after a hysterectomy. The healing period and long-term results might be significantly impacted by the type of hysterectomy used.
Different Techniques
In comparison to laparoscopic or vaginal hysterectomy, the recovery time for patients who have an abdominal hysterectomy might be longer and more painful. Patients may feel swelling, bruising, and pain at the location of the incision, and they may need to refrain from heavy activity for a few weeks.

Patients frequently feel less postoperative pain and a quicker return to regular activities following laparoscopic and vaginal hysterectomies. These operations could, however, come with dangers and issues include vaginal bleeding, infection, vaginal discharge, and bladder or bowel damage.
Vaginal hysterectomy and laparoscopic assisted vaginal hysterectomy can result in vaginal vault prolapse, while laparoscopic hysterectomy can result in gas pain, nausea, and shoulder pain.
Different Types
Partial hysterectomy
The outcome after four months can vary depending on the type of hysterectomy performed. Partial hysterectomy (Subtotal and Laparoscopic supracervical hysterectomy), which involves removing only a portion of the uterus, may have less impact on hormonal changes and sexual function than total or radical hysterectomy.
However, it’s important to note that every woman’s experience may differ. In general, recovery from a partial hysterectomy may be shorter and less painful than recovery from a total or radical hysterectomy.
After 4 months, women who have undergone a partial hysterectomy may experience some discomfort or pain in the pelvic area (easily manageable with pain medication if necessary), but this should be mild and typically goes away within a few weeks. Scar tissue may have formed by this point, but it’s usually not noticeable and shouldn’t cause any issues.
After a partial hysterectomy, many women report no noticeable alterations during sexual intercourse. Some women may suffer dryness or changes in libido can be treated with lubricants or hormone therapy.
Total hysterectomy
Whether or not the ovaries were also removed during a total hysterectomy may impact the results at 4 months. Ovarian preservation may result in less severe hormonal changes and menopausal symptoms for women.
Women may experience more severe hormonal changes, such as hot flashes, nocturnal sweats, and vaginal dryness if they have had their ovaries removed.
In terms of recovery, women who have undergone a total abdominal hysterectomy may experience more pelvic pain and discomfort than those who have had a partial hysterectomy. It may take longer to regain full mobility and return to normal activities and women may need to avoid certain activities for a more extended period of time.
Radical hysterectomy
For radical hysterectomy (sometimes recommended as part of cervical cancer treatment), which involves the removal of the uterus, cervix and surrounding tissue, recovery after 4 months may still be ongoing.
Women may experience discomfort or pain in the pelvic area, light vaginal bleeding, pelvic floor weakness as well as potential complications such as bladder or bowel movements issues.
Scar tissue may have formed by this point, but it may still be noticeable and potentially cause discomfort.
In terms of sexual function, women who have undergone a radical hysterectomy (whether laparoscopic, vaginal, or abdominal hysterectomy)) may experience changes in libido, as well as potential difficulties with dryness or tightness in the vagina.
However, it’s important to note that every woman’s experience may differ, and many women report no significant changes after this type of surgery.
Emotional Recovery
After undergoing a hysterectomy, many women experience a range of emotions, including depression, anxiety, anger and frustration.
The emotional challenges that arise after a hysterectomy can be linked to several factors, including the loss of reproductive organs, changes in hormone levels , and the underlying medical condition that necessitated the surgery.
Women who have undergone a hysterectomy due to cancer may experience additional emotional challenges, such as fear of recurrence or feelings of guilt. It is essential to remember that each woman’s emotional recovery journey after a hysterectomy is unique.
While some women may feel relieved, others may experience a sense of loss or grief. It’s crucial to seek support from loved ones, friends or a therapist who can help navigate the emotional rollercoaster.
Hormone Replacement Therapy after Hysterectomy
The removal of a woman’s ovaries during a hysterectomy might result in surgical menopause. When a woman’s body enters menopause following the removal of her ovaries, this is known as surgical menopause.
Numerous medical and psychological problems, including as dryness, mood swings, and hot flashes, may occur from this.
Women may be advised to use HRT to address these symptoms. After menopause, the body stops producing certain hormones, therefore HRT entails taking medication to replace them. HRT can be taken orally or applied topically using patches, gels, creams, and pills.
Other Gynecologic Surgeries and Emotional Recovery
Hysterectomy is not the only gynecologic surgery that can impact a woman’s emotional well-being. Other surgeries, such as oophorectomy (removal of the ovaries) and salpingectomy (removal of the fallopian tubes), can also lead to emotional challenges.
Women who undergo these surgeries may experience a sense of loss or grief, particularly if they were hoping to conceive in the future.
It is important to recognize that emotional recovery is a crucial part of the healing process after gynecologic surgery. Women who experience emotional distress after surgery should not hesitate to seek support from a therapist or counselor.
Menopausal Symptoms After 4 Months
After surgery, many women experience menopause symptoms. These indicators can cause a woman extreme discomfort and diminish her quality of life. There are numerous treatment options for menopausal symptoms after a hysterectomy.
Hormone replacement therapy (HRT) is a popular treatment option. Estrogen and occasionally progesterone are administered during HRT to replace hormones that the ovaries would normally produce.
Menopausal symptoms such as heat flashes and vaginal dryness can be alleviated by HRT. However, it is essential to bear in mind that HRT may not be suitable for all women , especially those who have previously experienced breast cancer or blood clots.
Another treatment option for menopausal symptoms after a hysterectomy is non-hormonal therapies.
These may include lifestyle changes, such as increasing physical activity and avoiding triggers that may cause hot flashes or medications such as antidepressants and anti-seizure drugs, which have been shown to be effective in managing hot flashes.
It’s also important to consider the emotional and psychological impact of menopausal symptoms after a hysterectomy. Women may experience feelings of loss, grief, and anxiety as they adjust to the changes in their bodies and cope with the symptoms of menopause.
Seeking support from loved ones, joining a support group or talking with a mental health professional can all be helpful in managing the emotional and psychological aspects of menopause after a hysterectomy.
Sexual Health After 4 Months
Many women may be concerned about how a hysterectomy will affect their sexual health. The reality is that the answer depends on a number of variables.
The type of hysterectomy executed is among the most significant factors.
Women who have undergone a total hysterectomy (removal of the uterus and cervix) will likely experience more significant sexual health changes than those who have undergone a partial hysterectomy (removal of the uterus only).
Women frequently have some vaginal bleeding, discomfort and vaginal discharge in the first few weeks or months following a hysterectomy. Sexual activity may become painful or uncomfortable as a result.
However, many women discover that their sexual function returns to normal after the first healing phase has gone. In fact, some women even claim that their sexual function has improved since their hysterectomy because they are no longer bothered by illnesses like endometriosis or uterine fibroids.
Intimacy tips and communication strategies
It’s crucial to discuss any changes you may be going through with your partner right away. This may involve both emotional and physical changes, such as a decrease in sexual desire or dryness. Building trust and closeness in your relationship can be facilitated by being open and honest with your partner.
Using a water-based lubricant during sex might assist ease any discomfort brought on by vaginal dryness in terms of physical changes. Additionally, since the risk of STDs may rise following a hysterectomy, it’s critical to engage in safe sexual behavior.
Discussion of alternative sexual practices
However, having a hysterectomy does not automatically indicate that your sexual life would suffer.
Vaginal penetration is simply one of many alternative sexual behaviors that can be pleasurable. Oral sex, shared masturbation, and sensuous massage are a few examples. It all comes down to figuring out what you and your partner can live with.
The most crucial thing is to practice patience with both your partner and yourself as you traverse this new stage of your life. Don’t be scared to experiment and look into new avenues for interpersonal communication. You can continue to have full and satisfied sex life after hysterectomy with open communication and a willingness to try new things.