Less Pain, More Precision: Why Robotic Hysterectomy is Worth Considering
What is Robotic Assisted Laparoscopic Hysterectomy?
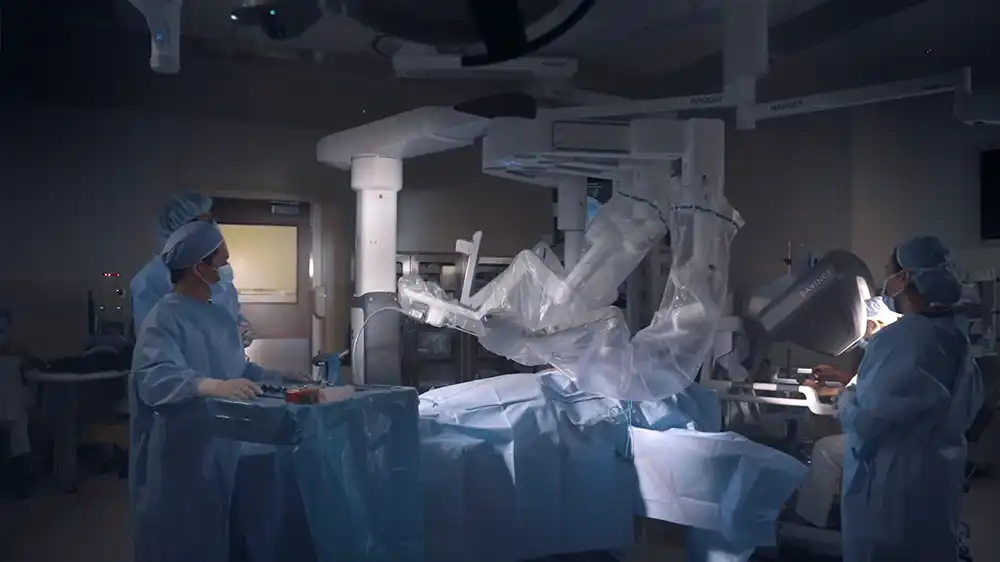
This type of laparoscopic hysterectomy is a minimally invasive surgical procedure that removes the uterus using a sophisticated robotic system. The robot-assisted system includes a surgical console and robotic limbs that with other surgical instruments are inserted through small abdominal incisions (instead of one large incision).

The surgeon sits at the console, which provides a high-definition, three-dimensional view of the surgical area.
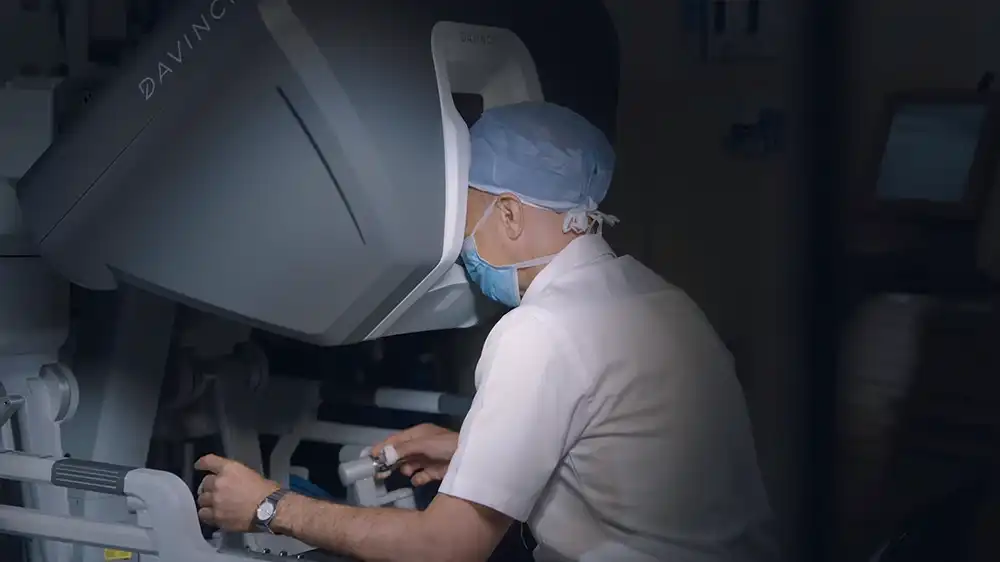
The surgeon manipulates the robotic limbs using hand and foot controls located on the console. These limbs contain specialized instruments such as scissors, forceps and a camera.

The camera provides a magnified view of the surgical site, enabling the surgeon to observe minute details that may not be visible to the unaided eye. The system includes sophisticated software that improves the control of the robot’s movements steadily, avoiding tremors.
How it’s performed
The procedure typically takes around 2-3 hours to complete and is performed under general anesthesia. The patient lies on the operating table, and several small incisions are made in their abdomen. The number and placement of these incisions depend on their specific needs and anatomy.
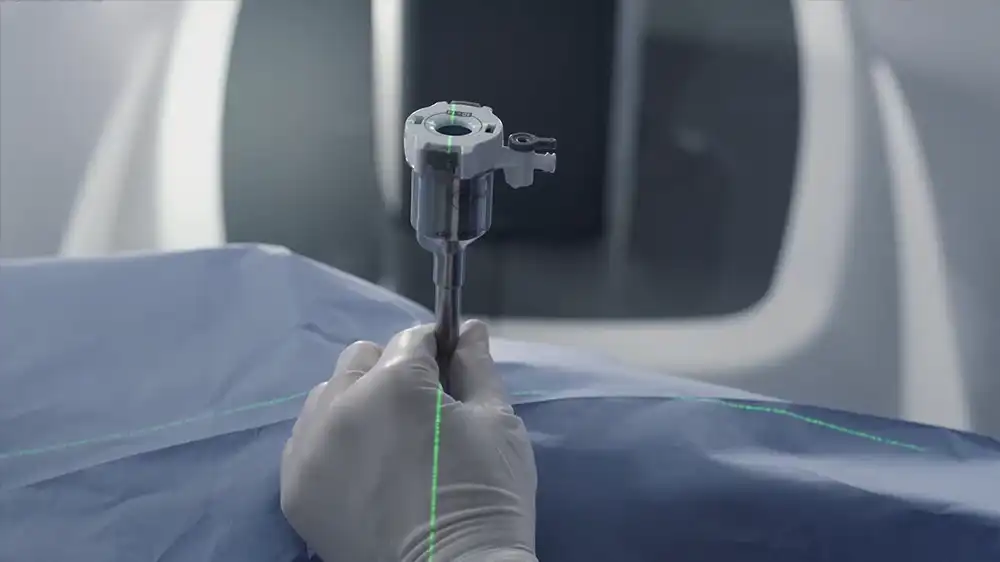
The system used for this procedure includes a surgical console, robotic arms that are inserted through the abdominal incisions, specialized surgical instruments such as scissors and forceps, and a camera. The console provides a high-definition, three-dimensional view of the surgical area which allows the surgeon to control the robotic arms with hand and foot controls. These instruments offer greater dexterity and flexibility than human hands, making it possible for the surgeon to make precise movements within tight spaces in the body while avoiding damage to surrounding organs or tissues.

Robot assisted hysterectomy vs. Abdominal or Vaginal Hysterectomy
Differences between the procedures
Robotic assisted laparoscopic hysterectomy offers several advantages over other types of hysterectomies, including abdominal hysterectomy and vaginal hysterectomy. With a minimally invasive hysterectomy involving only small incisions in the abdomen, patients experience less pelvic pain, scarring, and a quicker recovery time than with open surgery (partial hysterectomy, total hysterectomy or even radical hysterectomy). Additionally, robotic hysterectomy enables greater precision and control of surgical instruments than even conventional laparoscopic surgery, leading to fewer complications and less blood loss.
The robotic instruments also provide greater dexterity and flexibility than human hands, allowing the surgeon to make precise movements and minimize damage and posterior scar tissue. This is particularly important for the surgical removal of the uterus (and ovaries and fallopian tubes if required), as it requires delicate maneuvering to avoid damage to surrounding organs and tissues.

Which method is more cost-effective?
It depends on several factors, including the patient’s individual case, the hospital’s pricing and insurance coverage. Generally, a robotic assisted hysterectomy will cost more due to the technology and equipment required. However, it may be worth the cost if it results in a faster recovery and fewer complications.
It’s also important to consider the long-term cost-effectiveness of each procedure. While a traditional hysterectomy may be less expensive initially, there may be additional costs associated with complications, longer hospital stays, and extended recovery time. A minimally invasive option like RAH, may result in a faster recovery and fewer surgical risks, ultimately saving money in the long run.
Preparation for Robotic Hysterectomy
Necessary medical evaluations
Necessary Medical Evaluations: Before undergoing a robotic surgery, your healthcare provider will request a series of medical evaluations to ensure you are a suitable candidate for the procedure. These evaluations may include:
- Blood tests to check your blood type, hemoglobin, and clotting ability.
- Imaging scans such as ultrasounds, CT scans or MRIs to evaluate your pelvic anatomy and identify any abnormalities.
- Physical examinations to assess your overall health including your heart and lungs.
Your healthcare provider will review the results of these evaluations and determine whether or not you are a good candidate for the surgery.
Preoperative instructions
- It’s crucial to maintain fasting for at least 8 hours before surgery, including food, drinks, and even chewing gum. The objective here is not just to ensure an empty stomach but also to reduce the risk of pulmonary aspiration during anesthesia.
- Inform your surgeon about any medications or supplements you are taking, including dosage and frequency. Some medications may interact with anesthesia, bleeding, or other aspects of the surgery..
- Avoid smoking and alcohol consumption for at least a week before surgery, as they can cause complications such as bleeding, wound healing problems, and infections. In addition, nicotine and alcohol can interfere with anesthesia and may affect the metabolism of painkillers.
- It’s critical to arrange for someone to drive you home after the surgery and stay with you for a few days. You may feel groggy, dizzy, or nauseous after anesthesia, and your doctor may advise you to avoid driving or any physical activity for a while.
What to expect on the day of the surgery
As the day of your robotic-assisted hysterectomy surgery approaches, you may have many questions and concerns. What happens on the day of the surgery? What should you expect? Here’s a rundown of what typically happens.
Arrival
You will arrive at the hospital and check in with the receptionist. You will then change into a hospital gown and remove any jewelry, contacts, or glasses.
Checkups
A nurse will check your vital signs, such as blood pressure, pulse, and temperature, and start an IV line to give you fluids and medication. The nurse may also ask you some questions about your medical history and allergies.
Operating Room
You will be taken to the operating room, where the surgical team will prepare you for the surgery. They will apply sensors and monitors to your body to track your heart rate, oxygen levels, and other vital signs. They will also place a breathing tube in your mouth to help you breathe and administer anesthesia to make you unconscious.
Procedure
The surgical team will then perform the procedure using the robotic system and surgical tools, guided by your surgeon.
After Surgery
You will wake up in a recovery room, where the medical staff will monitor your vital signs and administer pain medication. You may experience some discomfort, cramping, or bloating, but your doctor will provide medication to alleviate these symptoms.
During the surgery
Steps involved in the procedure
Here’s a closer look at the steps involved:
Anesthesia: You’ll be given either general anesthesia, which will put you to sleep, or spinal anesthesia, which will numb the lower half of your body. Your anesthesiologist will talk with you about the best option for your situation.
Incision: Your surgeon will make a few small incisions in your abdomen to allow the robotic arms and camera to enter.
Robot Setup: The robotic arms and camera will be connected to a console where your surgeon will be seated. The surgeon controls the robotic surgical instruments movements with precision.
Uterus Removal: Using the robot’s arms, your surgeon will carefully remove your uterus and any other necessary tissues. The robotic arms allow for a minimally invasive procedure with less pain, scarring, and recovery time compared to traditional surgery.
Incision Closure: Your surgeon will close the small incisions with either stitches or surgical glue.
Recovery: You’ll be taken to the recovery room after the surgery, where you’ll be monitored.
Potential surgical risks and complications
While some risks, such as hemorrhage, infection, and anesthesia complications, are similar to those of conventional hysterectomy procedures, there are unique risks associated with a robotic assisted surgery that must be considered.
One of the most significant risks is the possibility of burns or electrical injuries from the surgical instruments, which can result from improper use or malfunction of the robotic arms. This risk is increased when there is insufficient training or experience with the system or when the system is used on patients who are not suitable candidates for the procedure.
A further risk to be aware of is the possibility that the robotic arms or console will malfunction or fail, which could result in procedure delays or the need for traditional surgery.
Candidacy for Robotic Hysterectomy
The majority of women who qualify for traditional hysterectomy surgery also qualify for this minimally invasive surgery. This includes women suffering from fibroids, endometriosis, uterine cancer or cervix cancer. However, a number of additional factors must be considered:
Women who are in excellent overall health and have no underlying medical conditions
Women with complex conditions, such as large fibroids or extensive endometriosis, may require a more conventional surgical approach.
Age and reproductive status: Women who are menopausal or postmenopausal and no longer intend to have children are generally excellent candidates for the procedure.
The size and shape of a woman’s uterus can also play a role in determining whether or not she is a suitable candidate for robotic assisted surgery. Women with extremely massive uteruses may require a more conventional surgical approach.
Cost
The location of the hospital, the kind of treatment necessary, the surgeon’s charge and the patient’s insurance coverage will all impact the procedure’s final cost. Yet it’s crucial to remember that the price of the robotic technology is not the only factor in determining the cost of the operation. Additional elements like preoperative tests and hospital stays may also influence the final cost.
Patients should typically budget between $10 000 and $30 000 or more for a robotic assisted hysterectomy procedure.
FAQ
How long does it take to recuperate from a robotic hysterectomy?
Depending on the patient, the recovery from a robotic hysterectomy may take anywhere from one to two days in the hospital to a few weeks of rest and minimal exercise.
How does a robotic hysterectomy differ from an open procedure?
In comparison to open surgery o other minimally invasive approaches, robotic hysterectomy has a number of benefits, including smaller incisions, less pain and blood loss, a shorter hospital stay, and a quicker return to normal activities. Moreover, robotic surgery gives the physician more control and precision lowering the risk of damaging surrounding tissues.
Will I have to adhere to a special diet before the procedure?
To make sure your digestive system is clear before the surgery, you’ll probably need to adhere to a specific diet. You will be given detailed instructions to follow by your surgeon.
How should I get ready for the procedure?
Follow carefully your surgeon’s instructions, which may entail stopping particular drugs, giving up smoking, and going without food or liquids for a specified amount of time prior to the procedure.
Will I be given anesthesia for the procedure?
Sure, you will receive general anesthetic so that you are sleepy and pain-free throughout the procedure.
