Mirena IUD vs. Hysterectomy: Treatment of Heavy Menstrual Bleeding
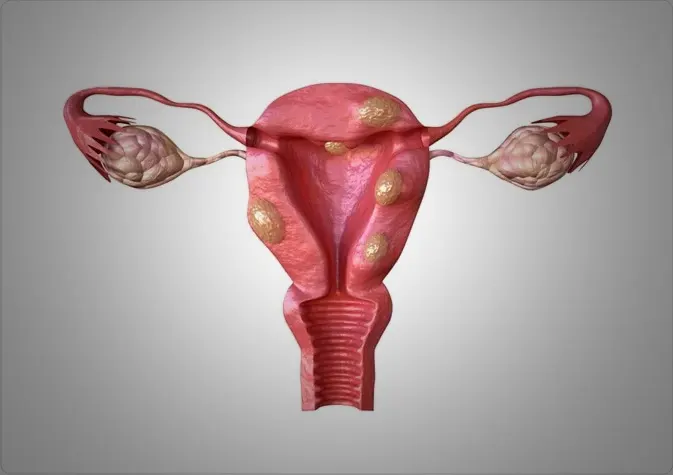
Heavy menstrual bleeding can significantly impact the quality of life for women, often requiring medical intervention for effective management. Two commonly considered treatment options for heavy menstrual bleeding are Mirena IUD (intrauterine device) and hysterectomy. This case study aims to compare these approaches, discussing their effectiveness, benefits, and potential drawbacks, ultimately providing insights into the decision-making process.
Understanding Menstrual Heavy Bleeding
Excessive or prolonged menstrual blood loss, medically termed as menorrhagia, is a condition that causes heavy menstrual bleeding. Women who experience this ailment often face challenges such as irregular bleeding patterns, severe pain, and anemia. It is imperative to identify appropriate treatment options to alleviate symptoms and enhance the overall well-being of those affected.
Mirena IUD: An Alternative to Hysterectomy
Mirena IUD and its Mechanism of Action
The Mirena IUD is a hormonal intrauterine device that releases levonorgestrel, a type of progestin, directly into the uterus. This hormone helps reduce menstrual blood flow by thinning the endometrial lining and suppressing its growth. The convenience of long-lasting contraception and potential benefits in managing heavy menstrual bleeding make Mirena an attractive option for many women.
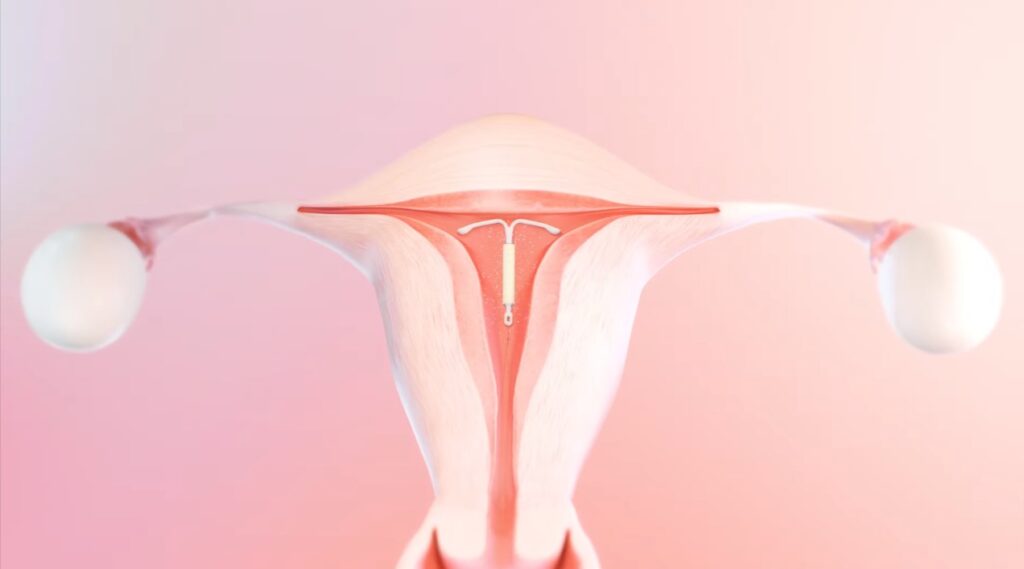
Effectiveness of Mirena IUD in Treating Heavy Menstrual Bleeding
Research studies have shown that Mirena IUD is an effective treatment for heavy menstrual bleeding. It offers a non-surgical alternative to hysterectomy and endometrial ablation for women seeking symptom relief. The levonorgestrel released by the IUD significantly reduces menstrual blood loss, leading to improved quality of life for many patients.
Comparative Analysis: Mirena IUD vs. Hysterectomy
Various factors should be taken into account to assess the appropriateness of Mirena IUD and hysterectomy as treatment options for heavy menstrual bleeding. These factors encompass treatment effectiveness, invasiveness, potential side effects, long-term outcomes, and cost-effectiveness.
Treatment Effectiveness
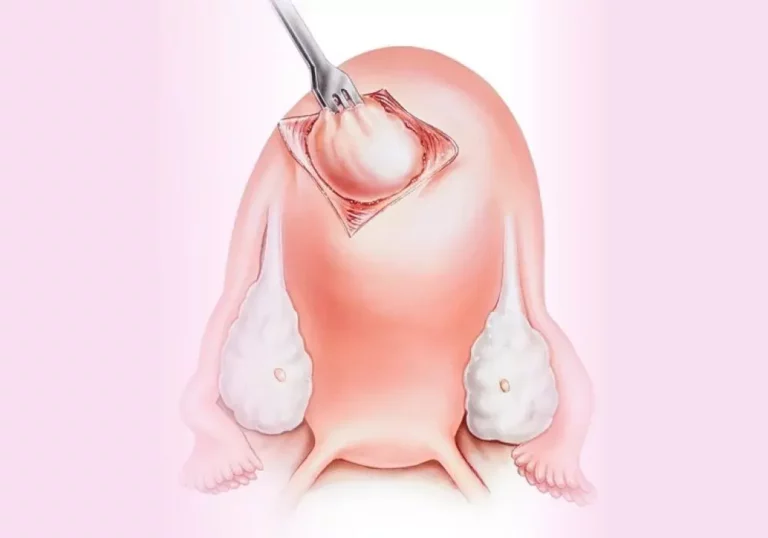
Research studies indicate that both Mirena IUD and hysterectomy offer effective treatment for heavy menstrual bleeding. Mirena operates by regulating hormones to reduce bleeding, while hysterectomy involves surgically removing the uterus, resulting in the cessation of menstruation. The selection between the two alternatives relies on individual circumstances, desired outcomes, and patient preferences.
Invasiveness and Side Effects
The insertion of Mirena IUD is a minimally invasive procedure that can be conducted on an outpatient basis. Common side effects may involve irregular bleeding during the initial adjustment period and the possibility of device expulsion. In contrast, hysterectomy is a significant surgical procedure that necessitates hospitalization, anesthesia,and a more prolonged recovery period. It is crucial to carefully consider potential complications associated with surgery and anesthesia.
Long-term Outcomes
Mirena IUD offers a reversible solution for heavy menstrual bleeding, and its effectiveness lasts for up to five years. Hysterectomy, however, is considered a definitive treatment as it permanently eliminates menstruation. The decision between the two depends on factors such as future fertility desires, severity of symptoms, and the overall health of the patient.
Cost-effectiveness Analysis
Evaluating the cost-effectiveness of Mirena IUD and hysterectomy is essential. While Mirena may have higher upfront costs associated with device insertion, it offers a cost-effective solution over time. Hysterectomy, on the other hand, may involve higher initial expenses but eliminates the need for ongoing contraception and follow-up appointments.
Endometrial Ablation for Heavy Menstrual Bleeding
Understanding Endometrial Ablation
Endometrial ablation is a non-surgical procedure employed to address heavy menstrual bleeding. It aims to reduce or eliminate menstrual periods by removing or destroying the endometrium, which is the lining of the uterus. Various techniques can be utilized for endometrial ablation, such as thermal balloon ablation, microwave ablation, and impedance-controlled bipolar radiofrequency ablation.
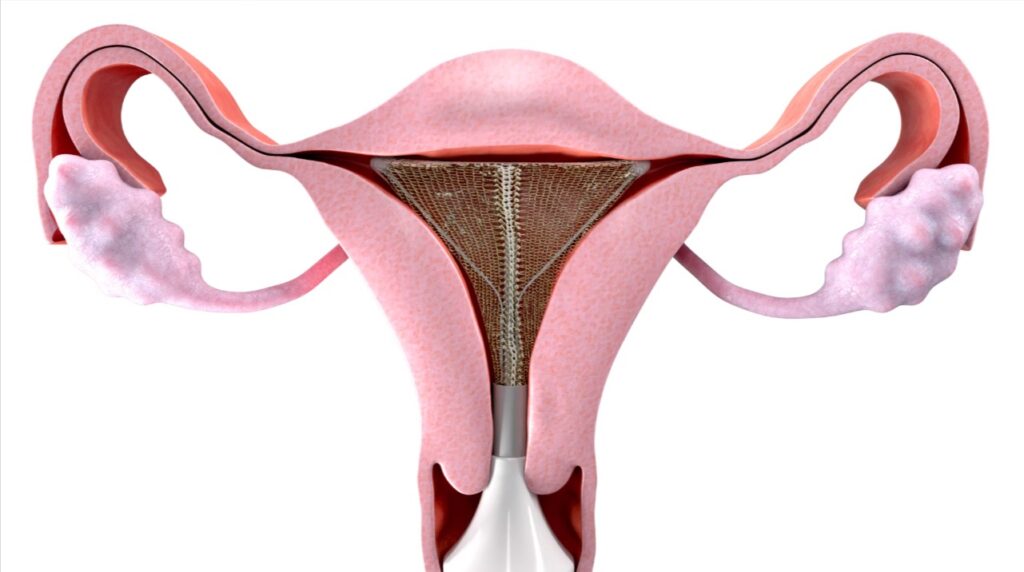
Effectiveness of Endometrial Ablation for Heavy Menstrual Bleeding
Endometrial ablation has demonstrated encouraging outcomes in the treatment of heavy menstrual bleeding. Research studies indicate that it can substantially lessen menstrual blood loss and alleviate symptoms in numerous women. However, it is important to note that endometrial ablation is typically recommended for women who do not intend to conceive in the future.
Comparative Analysis: Endometrial Ablation vs. Hysterectomy
When considering endometrial ablation and hysterectomy as treatment options for heavy menstrual bleeding, various factors come into play.
Treatment Effectiveness
Both endometrial ablation and hysterectomy have been shown to effectively reduce heavy menstrual bleeding. However, hysterectomy is considered a more definitive treatment as it involves the complete removal of the uterus, eliminating menstruation altogether. Endometrial ablation, although highly effective, may require additional treatments or follow-ups in some cases.
Invasiveness and Side Effects
Endometrial ablation is a minimally invasive technique that is frequently conducted on an outpatient basis, offering a quicker recuperation period when compared to the more extensive surgical procedure of hysterectomy, which necessitates hospitalization. Like any medical intervention, both procedures carry potential side effects, and it is advisable to have a thorough discussion with a healthcare professional to address any concerns.
Long-term Outcomes
Hysterectomy provides a permanent solution to heavy menstrual bleeding since it involves the removal of the uterus. In contrast, endometrial ablation may require further treatments or alternative interventions in the future if the symptoms persist or recur. Factors such as future fertility desires, severity of symptoms, and overall health must be considered when choosing between the two options.
Cost-effectiveness Analysis
Cost-effectiveness is an important consideration when evaluating treatment options for heavy menstrual bleeding. Hysterectomy involves higher initial costs due to surgery and hospitalization. However, it eliminates the need for ongoing contraception and follow-up appointments. Endometrial ablation may have lower initial costs, but additional treatments or interventions, if required, can increase the overall expenses over time.
Conclusion
When addressing heavy menstrual bleeding, several treatment options are available including Mirena IUD, endometrial ablation, and hysterectomy. Each option has its own benefits and considerations, and the choice should be made in consultation with a healthcare provider. Mirena IUD provides a non-surgical and reversible option, while endometrial ablation offers a minimally invasive procedure. Hysterectomy, on the other hand, provides a definitive solution by removing the uterus.
Understanding the individual’s symptoms, desires for future fertility, overall health, and cost considerations are crucial when determining the most appropriate treatment approach. By weighing the benefits and potential drawbacks of each option, women suffering from heavy menstrual bleeding can make informed decisions that best suit their unique circumstances, leading to improved quality of life and symptom management.
FAQs
How does endometrial ablation for menorrhagia compare to other ablative techniques?
The primary objective of endometrial ablation for menorrhagia is to diminish excessive menstrual bleeding. This procedure encompasses diverse techniques, including thermal balloon ablation, microwave ablation, and endometrial laser ablation.
What do studies suggest about the effectiveness of Mirena and hysterectomy for heavy menstrual bleeding?
Research findings suggest that both Mirena and hysterectomy are efficacious in managing heavy menstrual bleeding. Nevertheless, the selection between these two options relies on individual considerations such as patient preferences, medical background, and desired results.
What are the advantages of Mirena compared to hysterectomy for heavy menstrual bleeding?
Mirena offers certain advantages over hysterectomy, such as being a non-surgical option, reversible, and generally associated with fewer risks and complications. It provides a long-term contraceptive effect in addition to managing heavy bleeding.
Is there a reduction in bleeding with Mirena use?
Yes, Mirena use has been associated with a reduction in menstrual bleeding for many women. It releases a low dose of levonorgestrel hormone, which can help thin the endometrial lining and reduce bleeding.
How does the cost of hysterectomy compare to Mirena for the treatment of heavy menstrual bleeding?
In terms of the incremental cost, studies suggest that hysterectomy tends to dominate over Mirena when it comes to the initial expenses. However, the long-term costs should be based on the best available evidence, taking into account factors such as follow-up visits, potential complications, and individual patient needs.
What are the differences in the Institute for Health and Clinical Excellence (NICE) guidelines regarding Mirena, hysterectomy, and other treatment options for heavy menstrual bleeding?
The NICE guidelines provide recommendations for managing heavy menstrual bleeding, considering various interventions including Mirena, hysterectomy, and alternative treatments. These guidelines are based on a comprehensive evaluation of clinical effectiveness, safety, and cost-effectiveness.
What is the role of microwave and thermal balloon endometrial ablation in managing heavy menstrual bleeding?
Microwave and thermal balloon endometrial ablation are alternative techniques used to treat heavy menstrual bleeding. These procedures aim to remove or destroy the endometrial tissue, leading to a reduction in bleeding. They offer potential benefits as minimally invasive options compared to hysterectomy.
Are women with heavy menstrual bleeding more likely to undergo hysterectomy or opt for Mirena?
Studies suggest that women with heavy menstrual bleeding are more likely to undergo hysterectomy compared to choosing Mirena or other conservative treatments. The decision depends on several factors, including the severity of symptoms, desire for fertility preservation, and individual patient preferences.