Ovary Pain After Hysterectomy: Understanding and Managing Pelvic Discomfort
Hysterectomy, a frequently performed surgical procedure on women, entails the removal of the uterus. It is often suggested to address a range of conditions, including pelvic sore, endometriosis, uterine fibroids, and specific gynecological cancers. Although many individuals find relief from their symptoms following this procedure, it’s important to acknowledge that some women may encounter ovarian sore after hysterectomy. This blog post aims to explore the causes, risk factors, and approaches to managing pelvic discomfort post-hysterectomy, with specific attention to issues related to the ovaries.
Understanding Pelvic Pain after a Hysterectomy
The Role of Ovaries in Pelvic Pain

The ovaries, essential organs for reproductive and hormonal health, are closely connected to the pelvic region. They produce hormones, including estrogen and progesterone, and release eggs during the menstrual cycle. While a hysterectomy involves removing the uterus, one or both ovaries may be preserved depending on the patient’s medical condition and surgical approach.
Ovarian Remnant Syndrome(ORS): A Possible Culprit
Ovary sore after hysterectomy can stem from ORS, a potential underlying cause. This syndrome arises when a small portion of ovarian tissue is inadvertently left behind during the surgery. These residual ovarian remnants may continue to function, resulting in pain and hormonal imbalances. Although rare, it is crucial to acknowledge this possibility when assessing pelvic sore after the operation.
Recurrence of Pain and Endometriosis
Recurrence of pain in women with endometriosis can be a challenging and distressing experience. Despite undergoing treatments and interventions, the persistent nature of endometriosis often leads to the return of symptoms and discomfort. The unpredictable nature of the condition, coupled with its complex underlying mechanisms, contributes to the high rates of recurrence. The regrowth of endometrial tissue outside the uterus can cause pain, inflammation, and the formation of adhesions often affecting the ovaries, pelvic sidewall, or other pelvic organs.
Ovarian Torsion: A Potential Complication
Although uncommon, ovarian torsion is a potential cause of post-hysterectomy ovarian sore after hysterectomy can stem from various factors, including conditions like endometriosis, adhesions, or ORS. Additionally, surgical procedures such as laparoscopic or abdominal hysterectomy may contribute to pelvic aches due to the removal of organs and potential impact on the pelvic floor.pain. This condition occurs when the ovary twists on its own blood vessels, resulting in reduced blood flow and intense pain. Ovarian torsion can occur even after the uterus has been removed, particularly if one or both ovaries were preserved during the surgical procedure. It is crucial to be mindful of this possibility and promptly seek medical attention if you encounter sudden and severe pelvic sore following a hysterectomy.
Risk Factors for Ovary Pain after Hysterectomy
Several factors can increase the risk of experiencing pelvic sore after a hysterectomy. These include a history of endometriosis, severe pelvic sore prior to surgery, the presence of adhesions or scar tissue in the pelvic area, hormonal imbalances, and the preservation of one or both ovaries. It is important to discuss these risk factors with your gynecologist before undergoing a hysterectomy to set realistic expectations and explore potential management strategies.
Managing Pelvic Pain after Hysterectomy
Post-Operative Monitoring and Care
Following a hysterectomy, diligent monitoring and attentive post-operative care play a vital role in identifying and addressing any complications or lingering pain. Your gynecologist will likely advise regular check-ups and may prescribe imaging tests, such as a CT scan or MRI, to assess the pelvic region and ensure the absence of any underlying concerns.
Hormone Replacement Therapy and Menopause
In cases where both ovaries are removed during a hysterectomy or if the ovaries cease to function adequately, menopause can be induced, resulting in hormonal fluctuations. Hormone replacement therapy (HRT) might be essential to alleviate menopausal symptoms and regulate hormonal imbalances that can contribute to pelvic sore. It is advisable to have a thorough discussion with your healthcare provider about the available options for HRT.
Thoroughly discussing hormone replacement therapy (HRT) options with your healthcare provider is vital for determining the best treatment approach. HRT can alleviate symptoms like hot flashes, mood swings, and vaginal dryness, which contribute to pelvic discomfort.
Pelvic Floor Physical Therapy

Pelvic floor physical therapy offers a non-invasive solution for managing post-hysterectomy pelvic sore. This specialized therapy concentrates on strengthening and relaxing the pelvic floor muscles, which can become tense or weakened due to surgical procedures, hormonal fluctuations, or persistent pain. Collaborating with a skilled therapist can enhance pelvic muscle function and provide relief from discomfort.
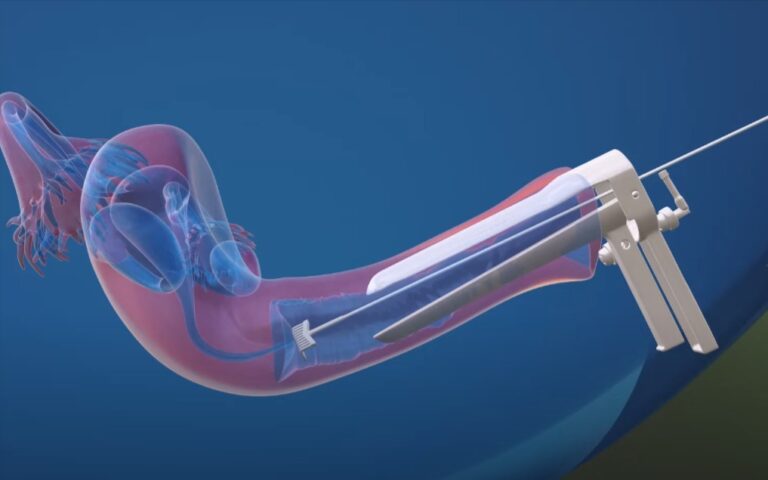
Surgical Intervention: Laparoscopy and Excision
If pain persists or reoccurs as a result of conditions such as endometriosis, ORS, or ovarian torsion, additional surgical intervention may be required. Laparoscopy, a minimally invasive procedure, can be employed to assess and address these conditions. Through laparoscopy, the surgeon gains visual access to the pelvic organs and can perform excision of any abnormal tissue or adhesions, thereby providing relief from pain.
Supportive Measures for Pain Management
For some women, pelvic sore after a hysterectomy may require a multidisciplinary approach to pain management. Along with medical interventions, there are various supportive measures that can be beneficial. These include:
- Heat therapy: Applying a warm compress or using a heating pad on the lower abdomen can help alleviate pelvic discomfort.
- Pain medications: Over-the-counter pain relievers or prescribed medications may be used to manage pain as recommended by your healthcare provider.
- Alternative therapies: Techniques such as acupuncture, chiropractic care, or massage therapy may provide additional pain relief and promote overall well-being.
- Emotional support: Dealing with chronic pain can take an emotional toll. Seeking support from friends, family, or joining support groups can provide a safe space to share experiences and gain emotional support.
Communicating with Your Healthcare Provider
It is crucial to maintain open and honest communication with your healthcare provider throughout the entire process. If you experience persistent or recurring aches after a hysterectomy, report your symptoms in detail to your gynecologist. Keeping a pain journal can be helpful, noting the location, intensity, and duration of pain, as well as any factors that may exacerbate or alleviate it. This information will assist your healthcare provider in determining the most appropriate course of action for managing your pain.
Conclusion
Although hysterectomy is known to alleviate certain gynecological conditions, it’s important to acknowledge that some women may encounter pelvic sore following the procedure. Understanding the potential causes, such as ORS, ovarian torsion, or recurrent endometriosis, and engaging in discussions about risk factors with your healthcare provider can help establish realistic expectations. By implementing appropriate management strategies, including post-operative monitoring, hormonal therapy, physical therapy, and surgical interventions when necessary, many women can discover relief from pelvic sore and regain their quality of life post-hysterectomy. It’s essential to remember that each person’s experience is unique, so collaborating closely with your healthcare team is crucial to determine the most suitable approach for your individual circumstances.
FAQs
Are there any other surgical interventions that can help with ovary pain after a hysterectomy?
When pain continues or returns after a hysterectomy, additional surgeries may be required. One such procedure is laparoscopy, which is minimally invasive. It can be used to assess and treat conditions such as endometriosis, adhesions, or ovarian cysts. Through laparoscopy, the surgeon can visualize the pelvic organs and perform necessary procedures like excision to alleviate the pain.
What are the common causes of ovary aches after hysterectomy?
ovarian sore after hysterectomy can stem from various factors, including conditions like endometriosis, adhesions, or ORS. Additionally, surgical procedures such as laparoscopic or abdominal hysterectomy may contribute to pelvic aches due to the removal of organs and potential impact on the pelvic floor.
What is ovarian remnant syndrome, and how does it relate to ovary aches after a hysterectomy?
ORS refers to the presence of residual ovarian tissue after a hysterectomy. These remnants can cause ovarian pain due to hormonal imbalances or the formation of cysts or adhesions. It is important to recognize this syndrome as a potential cause of post-hysterectomy pelvic pain.
What is considered abnormal pain after a hysterectomy?
Abnormal pain following a hysterectomy pertains to pain that exceeds normal levels, persists for a prolonged duration, or significantly hampers daily activities and overall well-being. This pain may manifest as sharp, stabbing, throbbing, or accompanied by additional symptoms like fever, excessive bleeding, or difficulty in urination. It is crucial to seek guidance from your healthcare provider if you encounter abnormal pain subsequent to a hysterectomy.
Can spasms contribute to ovary pain months after hysterectomy?
Spasms can be a contributing factor to ovarian pain that occurs several months after a hysterectomy. These spasms are involuntary contractions that can affect the pelvic muscles or residual scar tissue, resulting in discomfort. It is crucial to seek medical advice to undergo a thorough evaluation and receive personalized treatment for this condition.